Clare from Paignton, Devon, was a new mum to her 13-month-old son when she was diagnosed with a glioblastoma (GBM) in July 2022. For weeks she suffered with debilitating headaches and visual disturbances before a scan revealed the devastating news of a mass on her brain. The 36-year-old underwent surgery, radiotherapy and chemotherapy. After regrowth in November 2023, Clare is looking at experimental treatment to help prolong her life.

Clare tells her story…
My diagnosis has caused me to miss out on precious time with my two-year-old son, Teddy. I was a new to motherhood when I was told I had brain cancer in 2022. After my treatment, it took time to rebuild my relationship with Teddy having lost interest in being a mum when I was experiencing my symptoms and after invasive surgery. To think of how I was with him then, repulses me now.
Teddy was just 13 months when I started getting visual disturbances. It was a flashing of lights in my sight; a rainbow of colours shifted from my left to right eye, coming and going at the same time I experienced excruciating headaches.

Over six weeks, I went to my GP three times with a severe pain in my head and was given medication for migraines but that didn’t touch the sides.
“I was still taking paracetamol to control the pain and sleeping a lot. My relationship with Teddy began to deteriorate.”

I booked in for an eye test at Specsavers in The Willows in Torquay and described my symptoms to the ophthalmologist. I told them that every time I bent over I felt a surge of pain in my head and saw a flashing in my right eye. Tests revealed a defect in peripheral vision in my right eye. I was sent home with a letter for my GP to investigate further.
I felt as though people didn’t understand what I was going through. I was desperate to find out what was causing the immense pain in my head and changes in my vision.
I saw an acupuncturist in Paignton and for three days I felt some kind of relief. However a week later I found myself on the kitchen floor of my parent’s house. It was middle of the night and I couldn’t move my head from the floor, as if it was a magnet stuck to the surface. If I pressed my temples the pain eased enough for my mum to help me up and I went to A&E at Torbay Hospital.
A junior doctor looked at my eyes and saw something wasn’t right. Further tests discovered a mass on my brain and I was referred to Plymouth Hospital to be assessed.
Results of a scan confirmed I had a 6.4cm tumour on my brain. I was baffled. How was this not picked up sooner? The doctor told me the tumour displayed characteristics of a fast-growing and high-grade type and suspected that something unusual was detected in my eye test which is why I was referred to my GP.
“The neurosurgeon told me without surgery I would be dead by Christmas.”
I remember thinking, I’ve just had a baby, I want to be around to watch my son grow up for as long as I could.
I appreciated the honestly of the medical team. All the warnings that come with brain surgery; I wanted to hear those things, it felt like I had battled to get my diagnosis and it was only now that people were being honest. Whereas in hindsight, I think it was a lack of confidence and knowledge that medical practitioners I had seen before, had about brain tumours.
The wait for surgery was horrendous. The cancer had grown to 7cm in three weeks and I was slowly losing myself, acting out of character. I had already moved in with my parents and remember jumping out of a window because I didn’t want to speak to a neighbour. My cognition was impaired and I forgot I was a mum which meant Teddy spent more time with his dad and we drifted apart.
When I think back to that time, although my memory is hazy, I feel disgusted that I wasn’t there for Teddy. No-one tells you that as a parent you can feel a certain level of guilt in everyday life. You wonder if your child has enough food, are they warm enough? I had an extra level of this guilt; wondering if Teddy would inherit this disease and how he was going to grow up without his mum.
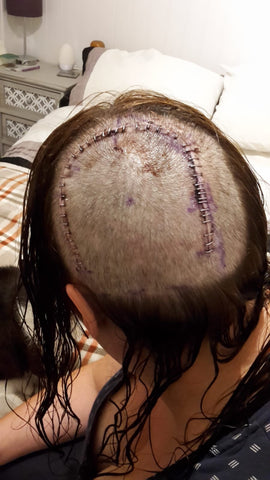
In August I had a six-hour operation at Derriford Hospital. Coming round in the hospital ward I was in agony. Screaming as I lay in bed. My vision was blurred and I couldn’t stand, I was sweating and felt isolated.
Two weeks later I returned home and doctors confirmed I had a grade 4 astrocytoma which is also classified as a glioblastoma (GBM). I’d already spent time before treatment started researching brain tumours.
“On hearing the pathology results I knew my life was over.”
A month later I began daily radiotherapy. Four days a week for six weeks I was to and from the hospital. A game of logistics which became intrusive on leading any kind of normal life following major surgery.
Chemotherapy ensued. I started on temozolomide which made me sick and I could only stomach a meal in the evening. At the same time I got to spend more time with Teddy and we were both getting to know each other again.

When my treatment finished in August 2023, the consultant gave me a prognosis of two to three years. I was grateful that my tumour was operable and that I had more time with my son.
I’d already made lifestyle changes and was following a keto diet which continues to help me with my focus. In September, after finishing NHS treatment, I started having vitamin C infusions; costing me £350 per session, which I have read is supposed to target the cancer cells.
In November a follow-up scan detected some regrowth, around 5mm which is about the size of a cheerio, and I decided to make the vitamin C infusions weekly rather than monthly.
In April I received results of my last scan (which took place in February) showing the mass now measuring 7mm, which is far below the growth rate my surgeon was expecting. My medical team is unsure why, and if there is one or a collective of treatments which can be attributed to this.
Despite my regrowth, I’ve been told that to qualify for another craniotomy my tumour must be a certain size as they aren’t sure if it scar tissue or the tumour.
“In all honesty, I’m not sure if another operation is something that I want due to the implications that comes with it.”
My eyesight is already compromised and my speech has been impacted. I’d rather opt for quality of life.
For brain tumour patients there are limited treatment options and the majority of those that are available are invasive and come with the threat of life-changing injuries. My own research has shown me there are clinical trial options abroad, but, for the majority of the working-class, this is an expense they simply can’t fund. I’m angry and frustrated.
Brain tumours is a disease that is horrendously underfunded when it comes to research. Since I was diagnosed, I’ve found myself constantly searching for other treatments. I want to support Brain Tumour Research so we can find kinder options for patients who receive this truly abysmal diagnosis.
For now, my treatment plan is ‘watch and wait’ and that feels torturous.
“My relationship with Teddy has blossomed and he now comes to me for hugs and I feel like his mum again.”
In May, he’ll be three and I’m very aware that could be the last birthday I get to spend with him. I don’t know if I’ll ever see him start school let alone do all the things that most parents take for granted.
Clare Smerdon
April 2024
Brain tumours are indiscriminate; they can affect anyone at any age. What’s more, they kill more children and adults under the age of 40 than any other cancer... yet just 1% of the national spend on cancer research has been allocated to this devastating disease since records began in 2002.
Brain Tumour Research is determined to change this.
If you have been inspired by Clare’s story, you may like to make a donation via www.braintumourresearch.org/donate or leave a gift in your will via www.braintumourresearch.org/legacy
Together we will find a cure

