Media Lawyer Rachel Boakes found out she could have a brain tumour at the same time as being diagnosed with thyroid cancer in February 2021. After undergoing two surgeries and radioactive iodine therapy to treat her thyroid cancer, Rachel, from Brixton, London, was informed she would need to undergo surgery for her brain tumour. She had an awake craniotomy in December 2021 after which it was confirmed she had a grade 2 astrocytoma. The 33-year-old is now being monitored with regular scans.

Rachel tells her story …
“My brain tumour journey started during the pandemic, in February 2021, when I went to see my GP about a small lump under my left ear.”
I’ve always been a bit of a hypochondriac, so when I noticed the lump I went to get it checked out, even though I suspected it was probably nothing. My GP asked me lots of questions, including whether my weight had changed lately and whether I ever had night sweats. I explained I had put on some weight (probably due to being so static and eating too much during the pandemic), and that I occasionally got hot at night but I assumed everyone experienced this and, again, thought it was probably nothing. When my blood test results came back, they showed I had elevated lymphocytes, which I was told could mean all sorts of things from the ordinary to the very worrying. Being cautious, we agreed I’d have an MRI scan to look into this further.
By the time I got my MRI result, the lump behind my ear was gone and I was told everything they were looking for as a result of that had come back clear. They did, however, make two incidental findings, inflammation of my thyroid and a lesion on my brain, but I was told not to worry as both could be nothing. I didn’t realise the word lesion meant tumour, so at the time I wasn’t aware they had found a brain tumour. I was referred to see an ear, nose and throat surgeon who felt my neck and told me I did, in fact, have a lump. It wasn’t very conspicuous at all.
“Again, I was told this could be nothing and was sent for more tests.”

In the meantime, I had another brain scan, which I was told would be repeated in six months’ time. After several attempts, the biopsies of my thyroid proved inconclusive and I was told there was a 50% chance I had thyroid cancer, with the only way to know for sure being to have surgery. As this happened during lockdown, I was given this information without my partner, Chris, beside me, which I found incredibly difficult. I was also unable to see friends or family during much of this time.
Having never had anaesthetic, the idea of having any surgery made me nervous but I knew it was the recommended next step, so I went ahead with it. It took a couple of weeks to get the results and, because of COVID-19 restrictions and, in part, my naivety, I was alone when I was told I had cancer in my thyroid and lymph nodes. This meant I would need another surgery and a type of radiotherapy known as radioactive iodine therapy, which involved me staying in isolation in hospital for three nights in June 2021.
“My radioactive levels were monitored and I was encouraged to drink a lot of water to help flush the chemical I was given through my body.”
I had another brain MRI in August 2021, six months after my first, to further investigate the lesion that had been found. I was at the Edinburgh Fringe with Chris when I got a call saying I might need to have brain surgery. I was told they still didn’t know what type of tumour I had, although it might be a low-grade glioma, but it would be discussed at a future multi-disciplinary team (MDT) meeting.
“At that point, nothing was said about me having a life-limiting or incurable condition.”

By September 2021, I had applied for a new job and so, during the interview process, I chased my neuro team to find out whether I was going to need brain surgery. I got a call back whilst Chris and I were in separate rooms as he had COVID and we were trying to avoid me catching it. This meant I was alone when I was given the news I needed surgery, and that it should happen in the next few months. I asked the doctor to confirm if I would be cured if the surgery went well. He said depending on the biopsy of my tumour, secondary treatment might be needed. I pushed again for more information and he finally said, for the first time, that if my tumour was what they suspected, there was no cure and it would be life-limiting. This was a huge shock. I then had to go and tell Chris the news, which felt as though it had come out of the blue and was the hardest thing I have ever done.
I decided to get a second opinion. One of my sister’s best friends was diagnosed with a glioblastoma (GBM) whilst he was living abroad and she had shared his scans with Mr Neil Kitchen, a neurologist at the National Hospital for Neurology and Neurosurgery (NHNN) in Queen Square. Having shown him my scans, he said I appeared to have a grade 2 astrocytoma. The surgeons I’d spoken to previously had different opinions on whether I should be awake or asleep for surgery and so, wanting to have as much guidance as possible, I sought the opinion of Professor Andrew McEvoy at the NHNN, because he does awake surgeries.
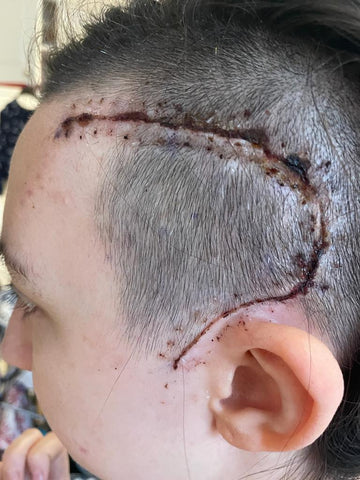
“After much deliberation, I decided to have an awake craniotomy with Prof McEvoy.”
It wasn’t an easy decision and we deliberated over it for a long time, with advice from friends and family. I was terrified about having brain surgery and the thought of being awake for it, and the possible emotional repercussions of that, scared me more. However, my tumour was in my left temporal lobe, the area that controls speech and language, so it was sensible to take a more cautious approach.
“I interviewed for my dream job the day before receiving the life-altering news about my tumour.”
I considered pulling out of the interview process but a friend convinced me to call and explain what was going on. When I did, I was encouraged to continue interviewing and see what happened. I was really surprised, and excited, when I got the job. It was amazing to receive some good news during a really dark period, and I think it helped motivate me in the run up to my surgery. My new employer offered to hold the role for me until I received my biopsy results.
In the meantime, I also started seeing a therapist who specialised in helping cancer patients. I don’t think I could have got through everything I’ve faced since then without her. She equipped me with lots of useful coping tools, recommending practical help from resources to read to prepare myself, to focusing on exercise we called ‘prehab’ in the run up to surgery, as well as giving me extensive emotional support.
Having also got engaged during this time, I partly distracted myself by planning our wedding. Chris and I found a venue we loved and we asked if they could hold the date on a good faith basis until I had got through my surgery and received my biopsy results. They said yes and I was blown away by their kindness. It makes such a difference when others give you hope.
“Small things like that are real gamechangers for people going through treatment.”

My surgery was booked for December 2021. Chris and I had to isolate for a week prior – our fourth isolation that year due to the different treatments I had – and say a lot of difficult goodbyes, which was really hard.
“My best friends did some amazing things during this time.”

My friend Lucy organised a surprise party for us, partly to celebrate our engagement but also so I could see as many people as possible before my surgery. I was completely surprised and hugely touched by all the work that went into this. It was an incredible evening that I still think about often. I wasn’t able to have any visitors in hospital due to COVID so my friend Elie created a visitor log and collated messages for me to read each day, so it would feel like they were with me, which was so special. And my friend Isabel, knowing how difficult I was finding the fact I was missing out on fun Christmas activities because of surgery, took the day off work so we could do Christmas things together, calling the day ‘Merry Boakesmas’.
Chris travelled to the hospital with me in a taxi – he accompanied me to every operation just to say goodbye. When I got there, I was on a busy ward and kept bumping into people who’d had a similar surgery to the one I was having, which was surreal. They were in different physical states and I found it very overwhelming. I had to arrive a day early to have a final scan and wasn’t allowed to go home due to the ongoing risk of COVID. I don’t think I slept at all that night due to nerves.
When I was woken up in theatre, the first thing I noticed was all the people in the room. As well as the surgeons and anaesthetist, I had a speech and language therapist who talked to me throughout. She was amazing, I don’t know how she kept me talking in that scenario. I was given drugs to keep me calm, which helped, but I had also prepared with my therapist beforehand having been warned some people panic during awake surgery. I really wanted to avoid this if at all possible, so I prepared as much as possible to try and stay calm.
“It all feels like a dream now.”
I only remember some of the things we talked about during the surgery, and being shown flash cards so my surgeons could see which parts of my speech and language might be affected by what they were doing. I remember the smell of the operating theatre and being told I was going to be put in an intra-operative MRI so my surgeons could be sure they’d got everything before closing me back up.
“When I was taken through to recovery, I couldn’t believe it was over.”
Being told everything had gone well was a huge relief, and I wanted to make sure they called Chris to let him know as soon as possible. We had set up a ‘telephone tree’ so after the hospital called him, he contacted my parents and a few friends, who contacted another friend and so on. I remember calling Chris and saying to him over and over again ‘I can’t believe the operation has happened’.

My sister Kate had been so integral to my journey that I wanted to be the one to call and let her know I was OK. She’s a barrister and was in chambers with two colleagues when I did. I think she was very shocked to receive a call from me so soon after surgery. It was a special moment to be able to speak to her.
“I also remember feeling very sick, not being able to eat much and feeling too wired to sleep.”
I tried listening to Harry Potter to help me sleep but wearing headphones proved difficult because of the massive bandage round my head. When I was able to return to the main ward, I appreciated being able to do simple things like brush my teeth.
“Looking in the mirror for the first time after surgery was interesting as I resembled the Mr Men’s Mr Bump character, bandaged and puffy and bruised.”
The woman opposite me was lovely so we chatted quite a bit and Kate dropped off healthy meals for me. I walked around with the physio team, checked in with my surgeons and met with my speech and language therapist. Then, after three days, I was allowed to return home, but it was strange how self-conscious I felt after getting my bandages off. I’m not usually bothered about my appearance but with my head swollen and my hair partly shaved, I felt I didn’t look like me, which was odd.
I was thrilled to be able to go home so quickly. I slept when I could and watched comfort TV, including lots of Christmas films. Slowly people started coming round but I found I couldn’t spend more than about 90 minutes with them without getting too tired. Lucy is a doctor so she helped me a lot after treatment, even helping to clean the blood from behind my ears. A few days later, about a week after surgery, I had a weird couple of hours where my speech went funny; I was having difficulty constructing sentences and didn’t feel like I was talking normally. I was told it could just be due to swelling so to relax for a while and see what happens.
“Thankfully, the doctors were right and my speech soon recovered.”
It took just over a month to get my biopsy results, which felt pretty quick considering Christmas and New Year fell in between. My tumour was confirmed to be a grade 2 astrocytoma. When I read about it further, it was hard not to panic given the stats and prognosis. I was told I’d be scanned every three months to check for any change and to just get on with my life as best as I could in between, which is what I’ve done. My scans have since moved to every six months.
“I was finally able to book my wedding and after eight weeks, which is as soon as I was allowed to, I started my new job.”
My confidence had taken a knock and I was nervous in case I wasn’t going to be able to do what I could before, but I knew the only way to find out was to give it a go. I started my new job about two months after surgery and, at first, I just worked half days, but I was full-time within three months. There was a brief period before I started where I experienced vertigo symptoms but that soon went away and, overall, I felt very well. I know I was lucky to recover so quickly and I’m now living a normal life, with a renewed appreciation for it.
It’s been two years since my tumour was removed and I feel really fortunate. I’m still able to work full-time and, as well as getting married, Chris and I have moved into a new house and made lots of amazing memories with friends and family.
My brain tumour is a huge part of who I am now. I think about it and what lies ahead multiple times a day. The reality of living with it hanging over me has been difficult to come to terms with but my amazing husband and my brilliant friends and family all help a huge amount, and I am continuing to see my therapist regularly.

“My advice for anyone going through this is to join support groups and try to speak to others who have been through it, connecting with them through charities, online or in your community.”
It’s so helpful to be able to have someone walk you through what to expect and recommend questions to ask your surgeon. Support groups are fantastic: brainstrust runs a brilliant online group for people with low grade gliomas that has been a huge help to me and there is a great Facebook group set up by the Astro Brain Tumour Fund for people with low grade gliomas where you can ask questions of other people going through treatment.
I would also recommend being very frank with friends and family about what you want or need them to do. Keeping busy is good, and making an effort to stay positive wherever possible. I find it harder than ever not to be a hypochondriac but I imagine most people have that after a cancer diagnosis. For everyone else, I would recommend talking. Too many people are scared to talk about brain tumours or they assume the patient won’t want to but in my experience that is rarely the case.
Rachel Boakes
April 2024
Brain tumours are indiscriminate; they can affect anyone at any age. What’s more, they kill more children and adults under the age of 40 than any other cancer... yet just 1% of the national spend on cancer research has been allocated to this devastating disease since records began in 2002.
Brain Tumour Research is determined to change this.
If you have been inspired by Rachel’s story you may like to make a donation via www.braintumourresearch.org/donate or leave a gift in your will via www.braintumourresearch.org/legacy
Together we will find a cure

